Guide by – Los Angeles Nursing Home Physical Restraint Attorney
 A Los Angeles nursing home physical restraint attorney at Cherepinskiy Law Firm will fight zealously to vindicate the rights of those patients whose freedom of movement, dignity, and autonomy had been stolen through the use of unwarranted physical restraints in the hands of nursing homes and assisted living facilities. In some cases, in order to prevent patients from injuring themselves or others, a physical restraint may become necessary. However, when physical restraints are used without a medical reason, excessively, without the consent of the patient or his / her responsible party, or just for the convenience of an assigned nurse or caregiver, this practice constitutes elder abuse. It is much easier to simply restrain an elderly patient than to provide the requisite attention and physical assistance, which is why understaffing of skilled nursing facilities is the leading cause of misuse of physical restraints.
A Los Angeles nursing home physical restraint attorney at Cherepinskiy Law Firm will fight zealously to vindicate the rights of those patients whose freedom of movement, dignity, and autonomy had been stolen through the use of unwarranted physical restraints in the hands of nursing homes and assisted living facilities. In some cases, in order to prevent patients from injuring themselves or others, a physical restraint may become necessary. However, when physical restraints are used without a medical reason, excessively, without the consent of the patient or his / her responsible party, or just for the convenience of an assigned nurse or caregiver, this practice constitutes elder abuse. It is much easier to simply restrain an elderly patient than to provide the requisite attention and physical assistance, which is why understaffing of skilled nursing facilities is the leading cause of misuse of physical restraints.
Pursuant to the California Elder Abuse and Dependent Adult Civil Protection Act (“EADACPA”), “physical abuse” includes the use of a physical restraint “[f]or any purpose not authorized by the physician and surgeon.” California Welfare & Institutions Code § 15610.63.
Unfortunately, skilled nursing facilities in California resort to the use of physical restraints at a rate, which is approximately 1.5 times higher than the rest of the United States. Similarly, assisted living facilities utilize physical restraints at an alarming rate. Essentially, California is facing an epidemic of physical restraint overuse in long-term care facilities.
The most common reasons for the inappropriate use of physical restraints are:
- For the staff’s convenience as opposed to patient or resident safety (e.g. to restrain patients or residents who have dementia or to avoid the need to periodically check on them);
- To compensate for the lack of sufficient staffing (understaffing); and
- For fall prevention (e.g. to prevent residents from falling out of bed).
Physical Restraints – Defined
California Code of Regulations (“CCR”), Title 22, § 72082 defines a physical restraint in the nursing home setting as: “any physical or mechanical device or material attached or adjacent to a patient’s body that the patient cannot remove easily, which has the effect of restricting the patient’s freedom of movement.”
Types of Physical Restraints
 Examples of physical restraints include the following:
Examples of physical restraints include the following:
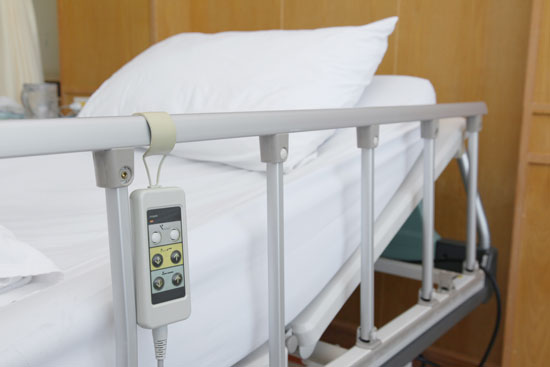
- Bed Rails;
- Belts;
- Soft ties;
- Vests;
- Hand mitts;
- Leg restraints;
- Arm restraint;
- Lap trays;
- Lap tables;
- Lap cushions;
- Special chairs with bars and belts;
- Positioning a wheelchair next to a wall to prevent the occupant’s movement; and even
- Bed sheets that are so tightly tucked in that it restrains the patient / resident’s movement.
Limitations on Use of Physical Restraints in Nursing Homes
California Code of Regulations, Title 22, § 72527, the Patients’ Bill of Rights, states that nursing home patients shall have the right:
- to be free from mental and physical abuse [CCR § 72527(a)(10)]; and
- to be free from physical restraints [CCR § 72527(a)(24)].
California Code of Regulations, Title 22, § 72319 limits the use of physical restraints at skilled nursing facilities as follows:
- A detailed order by a healthcare provider (e.g. a physician) is required before any restraints can be utilized [CCR §72319(b)];
- Restraints may not be used as punishment, for the staff’s convenience, or as a substitute for more effective medical and nursing care [CCR §72319(d)];
- Acceptable physical restraints are limited to cloth vests, soft cloth mittens, soft ties that do not to cause abrasions or restrict blood circulation, and seat belts and trays equipped with spring release mechanisms [CCR §72319(c)];
- They must be applied in a way that allows for a quick removal in case of a fire or other emergency [CCR §72319(h)]; and
- Restraints with locking devices and seclusion (e.g. locking patients alone in a room) are absolutely prohibited [CCR §72319(e) and (f)].
Further, pursuant to California Code of Regulations, Title 22, § 72528(a), if a physician orders the use of a physical restraint at a skilled nursing facility, the physician must obtain informed consent from the patient or the patient’s family. California Code of Regulations, Title 22, §§ 72528(c) and 72527(e)(1) [the Patients’ Bill of Rights] require that a nursing home verify that the physician actually did obtain informed consent for the use of a physical restraint. These regulations are very complicated and, when pursuing a case involving restraints, victims need the assistance of the Los Angeles nursing home physical restraint attorney who knows the applicable laws and regulations well.
Limitations of Physical Restraints in Assisted Living Facilities
California Code of Regulations (CCR), Title 22, § 87468 establishes the Personal Rights of residents at residential care facilities for the elderly (RCFE’s), also known as assisted living facilities. Based on CCR § 87468 (a)(3) and CCR § 87468 (a)(6), the residents’ rights include the following:
Mental Freedom Rights
The right to be free from:
-
- mental abuse
-
- humiliation
-
- corporal or unusual punishment
-
- intimidation or
-
- other actions, which are punitive in nature
The Freedom of Movement Rights
-
- the right to depart from or leave the facility at any time and
-
- the right to not be locked anywhere on facility’s premises (including buildings and rooms) at any time, including day and night.
This means that residents must never be locked in their rooms or prevented from going outside of the facility (e.g. by blocking exits, using door locks, etc.) Locking main doors at night or installing window bars for safety can be allowed with appropriate permits.
Postural Supports
The use of postural supports, including bed rails, is limited by California Code of Regulations (CCR), Title 22, § 87608. Specifically:
- CCR § 87608(a)(1) limits allowed postural supports to those devices and appliances, which are used to improve independent functioning and mobility, as well as provide appropriate balance and body positioning (e.g. soft ties, spring release trays, and braces). Such devices are allowed as long as they are not used to restrict residents’ movement;
- CCR § 87608(a)(1) explicitly prohibits the use of postural supports (such as bed rails) for “preventing a resident from falling out of bed”;
- CCR § 87608(a)(2) explicitly mandates that any postural supports must be fastened or tied in a manner that “permits quick release by the resident”;
- CCR § 87608(a)(5) says that postural supports may never be used to:
-
- tie patients; or
- deprive or limit residents’ use of their hands or feet;
- Pursuant to CCR § 87608 (a)(5)(A), “a bed rail that extends from the head half the length of the bed and used only for assistance with mobility shall be allowed”; and
- CCR § 87608 (a)(5)(B) completely prohibits the use of full-length bed rails (extending the entire length of the bed), unless the resident is receiving hospice care.
Bed rails (also called “side rails”) are especially dangerous for elderly residents of assisted living facilities, because they carry the heightened risk of entrapment and death. In April of 2010, the U.S. Food and Drug Administration (FDA) issued its revised “Guide to Bed Safety Bed Rails.” This document indicated that, during the 1985 – 2009 time-period, FDA received reports of multiple incidents where patients had been severely injured or killed in beds with side rails. The reports showed that these patients had been entangled, trapped, caught, or even strangled. There were 803 reported incidents. Of those incidents, 480 people – more than half – died because of bed rail entrapment. Most of the victims were elderly, frail, or confused.
The FDA Guide to Bed Safety Bed Rails stressed that most patients can be in bed safely without bed rails, and stated:
- “keep the bed in the lowest position with wheels locked”; and
- “when the patient is at risk of falling out of bed, place mats next to the bed, as long as this does not create a greater risk of accident”
Unfortunately, despite the detailed Title 22 regulations and the warnings by the U.S. Food and Drug Administration, California assisted living facilities continue to keep residents with impaired mobility unattended in hospital beds with side rails that are raised at all times. This reckless practice of abuse, utilized to prevent residents from falling out of bed, to restrain residents with dementia, or simply for the caregivers’ convenience, frequently leads to tragic outcomes and residents’ death. The Los Angeles nursing home physical restraint attorney at Cherepinskiy Law Firm is devoted to fighting on behalf of those elderly patients who fell victim to physical restraints.
Risks of Use of Physical Restraints in Elderly
The misuse and overuse of physical restrains in long-term care facilities can cause multiple significant injuries. The physical consequences of restraining elderly patients and residents include the following:
- Bed sores caused by prolonged periods of immobility;
- Pain and discomfort;
- Skin bruising (e.g. when patients attempt to free themselves);
- Muscle strength deficiency (muscular atrophy from lack of movement);
- Weakening of the cardiovascular system;
- Respiratory complications and the risk of aspiration pneumonia;
- Urinary incontinence;
- Constipation; and
- An increased risk of death (e.g. strangulation from bed rail entrapment or a fatal head trauma).
Also, victims of physical restraints exhibit an increased dependency upon nurses and caregivers in terms of activities of daily living. This factor, as well as the actual mental trauma of feeling restrained, lead to severe psychological consequences, including restlessness, agitation, depression, social isolation, as well as feelings of loss of self-respect, loss of dignity, and shame.
Avoiding Physical Restraints of the Elderly
Instead of humiliating elderly residents and patients and subjecting them to significant health and safety risks, assisted living facilities and nursing homes must:
- Use adequate staffing;
- Provide appropriate monitoring and supervision or patients / residents;
- Use low beds with floor mats;
- Provide physical therapy, occupational therapy, and encourage social activities;
- Provide appropriate therapy and attention to elderly individuals with mental health issues (e.g. dementia / Alzheimer’s); and
- Most importantly, place patient safety above staff convenience.
These measures may increase the cost of operation of long-term care facilities. If facilities choose money over the dignity, health, safety and lives of the people they are entrusted to care for, they commit elder abuse.
Take Action! Promptly Contact a Los Angeles Nursing Home Physical Restraint Lawyer for a Free Consultation
As the Los Angeles nursing home physical restraint lawyer, Dmitriy Cherepinskiy, and his firm, vigorously pursue justice. If you or your loved one fell victim of physical restraints, this firm will serve to fervently vindicate your rights. If physical restraints in the hands of an assisted living facility or a nursing home caused the death of a loved one, the Los Angeles elderly physical restraint lawyer at this firm will show compassion and will fight relentlessly in a wrongful death case.
If you suspect elder abuse in the form of physical restraints, please call or fill out an electronic contact form today to request a free consultation. Cherepinskiy Law Firm, the Los Angeles assisted living physical restraint lawyer, will work tenaciously to bring the wrongdoers to justice, and to obtain the maximum case value and compensation you deserve.
This firm fights for clients throughout California, including Los Angeles, Orange County, as well as Ventura, Riverside and San Bernardino Counties.
Source
1. “Use of physical restraint in nursing homes: clinical‐ethical considerations“, Journal of Medical Ethics (March 2006): https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2564468/
2. https://www.fda.gov/medical-devices/bed-rail-safety/safety-concerns-about-bed-rails